05 May We’ve got your Back
Think about this: Back pain is the number one cause of disability worldwide in people 25 to 64 years of age, and the United States is no different. A staggering 88 Billion of federal healthcare dollars are spent annually to diagnose and provide care for individuals with complaints of low back pain, and the outcomes are not improving. Much has been discussed recently of the resulting opioid epidemic, yet physicians continue to provide medication and offer diagnostic testing and surgical consults with generally poor outcomes. Conservative measures such as physical therapy, moderate exercise and lifestyle modifications have shown promise in returning patients to an active lifestyle. However, overall our healthcare system has continues to struggle to meet the needs of patients with low back pain.
Let’s consider these facts related to low back pain:
- Prolonged sitting and sedentary lifestyles are responsible for the underlying conditions related to many episodes of low back pain, and these are controllable circumstances for most individuals.
- Back pain is significantly more likely to become a chronic condition in individuals who are sedentary and in poorer health.
- MRI and x-ray findings are predictably abnormal in patients over 40 years of age. Findings of pathology on MRI and X-ray must be related to the present circumstances and symptoms of a patient to factor into treatment recommendations.
- Not all back pain is the same, therefore not all back pain responds to the same treatment. Research shows that if treatment is individualized and directed toward an individual’s characteristics, outcomes are much better. Some of the treatment clusters include:
- General and specific spinal mobility problems;
- Core and abdominal muscle strength deficits;
- Presence of abnormal postural strain, such as prolonged sitting and bending; and
- Specific movement and pain patterns that are matched together.
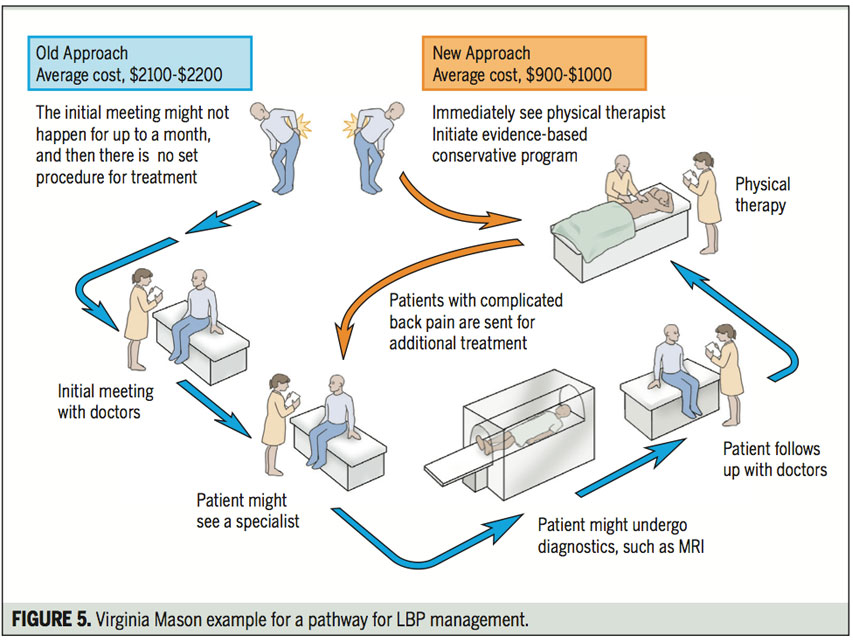
- The Virginia Mason Medical Center, working with Insurer Aetna, were able to dramatically shift the cost and burden of low back care by sending patients directly to physical therapy care, resulting in:
- Decreasing waiting times to see a provider from 31 days to one day
- A drop in MRI utilization from 42% to 6% of patients
- 94% of patients experienced no work loss,
- 73% of patients utilized no prescription medications, and
- A cost savings of approximately 50% for the patient
- Despite abundant evidence and published guidelines in the medical literature calling for conservative initial treatment of most back pain through methods including physical therapy and over-the-counter medications such as ibuprofen and acetaminophen, a study published in JAMA (Journal of the American Medical Association) Internal Medicine (“Worsening Trends in the Management and Treatment of Back Pain” – September 23, 2013) indicates that physicians often over-treat back pain, with increases in use of imaging, narcotics, and referrals to other physicians. The findings confirmed that the over-treatment leads to unnecessary expenses, and do not improve outcomes for patients.
In summary, back pain is overwhelmingly related to lifestyle and general health status; that wear and tear changes in the spine are normal with aging; that patients respond better to individualized care related to their specific movement and pain characteristics than to generalized care; and that earlier access to appropriate physical therapy returns patients to an active life faster and with lower costs.
Do you suffer from back pain? Often times engaging in a gentle to moderate exercise routine can improve strength and mobility, restoring full activity and health. If your program needs a nudge, let us know. We help hundreds of patients a month get back to an active life faster, and we’d love to assist you as well!
To your comfortable movement,
Brian